Travelling with Diabetes: A Complete 2026 Guide
Having diabetes shouldn’t stop you from travelling. Millions of people with diabetes enjoy holidays, city breaks, and family trips every year. What makes the difference between a stressful journey and a safe, enjoyable one is planning.
The good news is that travelling with diabetes is entirely manageable. You just need to take time to consider a few key issues before you go. This guide walks you through every step – from booking your trip to managing your condition in different climates and dealing with emergencies abroad.
Whether you’re flying to Spain, driving through Europe, or taking a cruise, the principles are the same: preparation, awareness, and confidence. Let’s start.
Travelling with Diabetes: Key Planning Steps
Ideally, start preparing for your trip four to six weeks before you depart. Use this alongside our travel health checklist for over-50s, which covers GP visits, vaccinations and packing essentials beyond diabetes care. This gives you time to arrange healthcare support, sort documentation, and gather supplies without stress.
Step 1: See Your GP
Make an appointment with your GP to discuss your travel plans. Your GP can:
- Advise on any necessary medication changes for your destination or travel duration
- Provide a letter confirming your diagnosis and treatment – this is essential for carrying syringes, insulin, and other equipment through airport security
- Give you a record of your medication names (both brand and generic) in case you need treatment abroad
- Suggest any vaccinations you may need
Note: some GPs charge for a letter (typically £20-£30). Check in advance.
Step 2: Check Insulin Availability at Your Destination
Contact your insulin manufacturer to confirm that your insulin is available in the country you’re visiting. Insulin types vary by country, and your regular brand may not be supplied under the same name abroad. This is crucial information to have before you travel.
If your insulin is not available, ask your GP whether you can bring enough for the entire trip. Most countries allow a reasonable personal supply.
Step 3: Arrange Travel Insurance
Travel insurance is essential when you have diabetes. Standard policies often exclude or limit cover for pre-existing medical conditions. You need specialist travel insurance that covers diabetes, emergency medical treatment, and hospitalisation.
Even if you’re travelling within the European Union and have a free European Health Insurance Card (EHIC), buy travel insurance as well. The EHIC covers necessary medical treatment but does not cover repatriation, cancellation due to illness, or private healthcare costs. For detailed guidance, see Diabetes UK’s travel insurance advice.
Step 4: Obtain an EHIC (EU Travel)
If you’re travelling to a European Union member country, apply for a free EHIC online at EHIC.org.uk. This entitles you to necessary medical treatment at the same cost as a local resident. It’s not a substitute for travel insurance, but it’s useful to have.
Step 5: Get a Diabetes Identity Card
Carry a card or wristband identifying you as someone with diabetes. In an emergency – especially if you become unconscious or confused – medical staff need to know immediately that you have diabetes. You can order these from Diabetes UK or buy them from high street chemists.
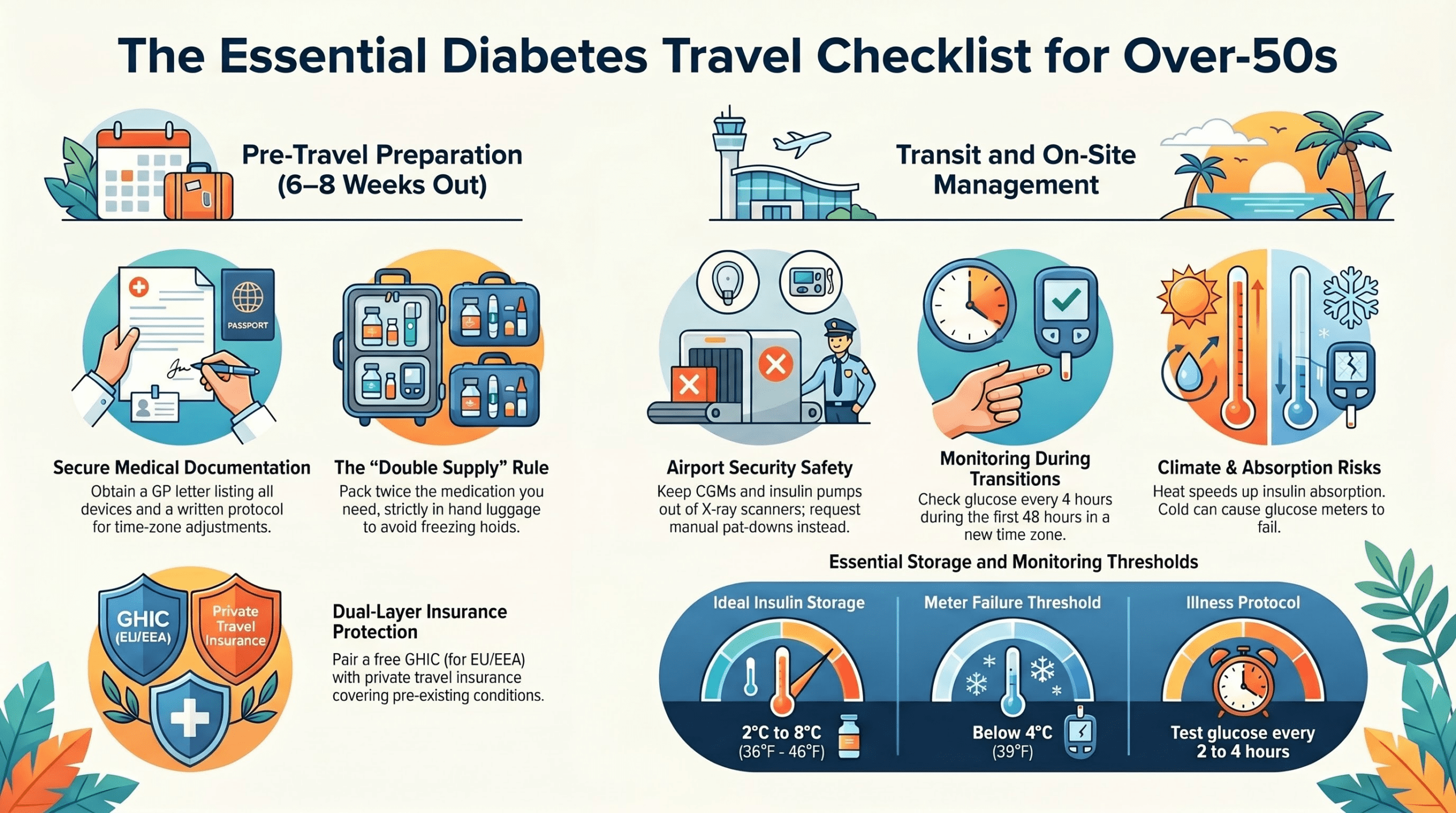
Your Pre-Trip Checklist: Insulin Pumps and Glucose Monitors
If you use an insulin pump or continuous glucose monitor (CGM), take extra steps before you fly:
- Contact your airline. Ask whether insulin pumps and CGMs are permitted during flight and whether they’re safe to pass through airport X-ray machines. Most modern devices are safe, but it’s best to confirm. Keep your device with you in the cabin – never pack it in hold baggage.
- Bring extra batteries and supplies. Airports and flights may delay or divert. Pack far more insulin pump supplies and CGM sensors than you expect to need.
- Carry a backup insulin pen or syringe. If your pump fails, you’ll need insulin as a backup.
- Inform security at the airport. Tell airport security staff that you’re wearing a medical device so they can visually inspect it instead of making you remove it.
Packing Your Diabetes Supplies
Proper packing protects your insulin and equipment from damage, loss, and temperature damage. For everything else you should pack alongside your diabetes supplies, see our essential travel first aid kit guide.
Storage and Protection
Pack your diabetes supplies in an airtight container or wrapped in bubble wrap, then wrap the whole bundle in a towel. Place it in the middle of your suitcase – not near the edges where it may be crushed or exposed to extreme temperatures.
If you’re flying, never pack insulin in hold baggage. Hold baggage is not temperature-controlled and insulin can be destroyed by extreme cold or heat. Keep all insulin and temperature-sensitive equipment in your carry-on bag.
Split Your Supplies
Divide your diabetes supplies between your checked luggage and hand luggage. If your checked bag is lost or delayed, you’ll still have insulin, testing strips, lancets, and syringes with you. This is one of the most important precautions you can take.
Supplies Checklist
- More insulin than you expect to need (ideally 1.5 times the amount)
- More test strips and lancets than usual
- Syringes or pens (plus spares)
- Glucose meter and batteries
- Glucagon emergency kit
- Fast-acting carbohydrates (glucose tablets, dextrose sweets, emergency snack bars)
- Your diabetes identity card and GP letter
- Insurance documents and travel insurance contact details
- Prescriptions or records of your medications (brand and generic names)
Flying with Diabetes
Air travel with diabetes requires a few specific precautions.
At Security
Inform airport security that you have diabetes and need to carry medicinal supplies. Have your GP letter and any device documentation ready. Security staff may test your insulin or equipment, so allow extra time at security.
If you’re wearing an insulin pump or CGM, tell security staff. They will visually inspect it rather than making you remove it or put it through an X-ray machine.
On the Plane
Keep your insulin and essential supplies in your hand baggage at all times. Some airlines require you to hand medication to cabin crew for storage in a cool area. If asked, confirm that insulin must be kept between 2-8C and cannot be frozen.
Insulin stored at room temperature (below 25C) is safe for short periods, but during a long flight, especially in a warm cabin, it can degrade. If the airline insists on storing insulin, confirm they’ll keep it refrigerated.

How Climate Affects Diabetes Control
Temperature changes affect both insulin absorption and blood glucose readings. Understanding these risks helps you stay safe in any climate.
Travelling to Hot Climates
Heat increases insulin absorption. Insulin absorbed too quickly can cause your blood glucose to drop unexpectedly, risking hypoglycaemia (hypo). Additionally, hot weather and sun exposure can raise your blood glucose naturally as your body burns energy managing heat.
What to Do:
- Monitor your blood glucose more often – at least four times daily, or as advised by your GP
- Check your insulin supplies are stored correctly. Use an insulated insulin travel pack if temperatures exceed 25C
- Adjust your insulin doses as advised by your GP if your levels run consistently high or low
- Stay hydrated – dehydration can make blood glucose harder to control
- Be aware that extreme heat can damage your glucose meter. Keep it in a cool, dry place
- Avoid prolonged sunbathing, as sun exposure and heat together can spike your glucose
Travelling to Cold Climates
Cold slows insulin absorption initially. This means insulin takes longer to work, which can cause high blood glucose. However, when you warm up indoors after being outside, insulin can be absorbed suddenly and cause a hypo.
Cold also increases the risk of hypos because your body uses more energy to stay warm. This extra energy use lowers blood glucose naturally.
Hypos are more dangerous in cold climates. When you have a hypo, your body’s natural response is to shiver and generate heat. But when your blood glucose is dangerously low, your body cannot generate heat effectively. This increases the risk of hypothermia – a life-threatening drop in core body temperature.
What to Do:
- Carry fast-acting carbohydrates (glucose tablets, sweets, energy bars) in your pockets at all times, not in a rucksack
- Check your blood glucose before and after time in the cold
- Keep your glucose meter warm – extreme cold can damage it and give false readings
- Wear a diabetes identity bracelet so people can help quickly if you have a hypo
- Tell travel companions how to recognise a hypo and where you keep emergency supplies
- Do not exercise in the cold without eating something first
Managing Illness Abroad
Illness while travelling can complicate diabetes control. If you are travelling to a tropical destination, also see our guide on avoiding insect bites and stings while travelling, as bite-related infections heal more slowly when blood glucose is unstable. The good news is that with the right approach, you can manage it safely.
If You Need Medical Treatment
Always tell any doctor or healthcare provider abroad:
- That you have diabetes
- Your current medication – both the brand name and the generic (chemical) name
- Any other conditions or allergies you have
- Your GP’s contact details
Carrying a list of your medications in both English and the local language can be helpful in non-English-speaking countries.
Sickness, Diarrhoea, and Vomiting
If you develop sickness, diarrhoea, or vomiting abroad – all common in unfamiliar climates or with unfamiliar food – do not stop taking your insulin. This is crucial. Many people worry that if they can’t eat, they shouldn’t take insulin. This is incorrect and dangerous.
Instead:
- Continue your insulin as prescribed. Your body still needs insulin to regulate blood glucose
- Try to maintain carbohydrate intake with drinks, broths, or foods you can tolerate (soup, rice, crackers, juice, fizzy drinks)
- Monitor your blood glucose every 2-4 hours. Illness can make your levels unpredictable
- Stay hydrated. Vomiting and diarrhoea cause fluid loss, which can worsen high blood glucose
- Seek medical help if you develop signs of diabetic ketoacidosis (DKA): fruity-smelling breath, rapid breathing, severe nausea, or drowsiness
Comparison Table: NHS vs Private Healthcare Abroad
If you need medical treatment while travelling, you may be offered NHS treatment (via EHIC in EU countries) or private healthcare. For full coverage of policy options, premiums and the disclosure rules every diabetic traveller should know, see our travel insurance with medical conditions guide. Here’s what you need to know:
| Aspect | NHS (with EHIC in EU) | Private Healthcare |
|---|---|---|
| Cost | Free or minimal (same as local resident) | Can be £100-£500+ per consultation |
| Waiting Time | May be 24-72 hours for non-urgent care | Usually same day or next day |
| Availability | Limited to EU member states; availability varies | Available worldwide in developed countries |
| Emergency Cover | Yes, for emergency treatment | Yes, if covered by your travel insurance |
| Best For | Emergency care in EU; reduces out-of-pocket costs | Quick non-emergency treatment; routine follow-up |
Key Takeaways
- Plan four to six weeks ahead. See your GP, arrange insurance, and gather documentation
- Always carry insulin in hand baggage. Hold baggage is not temperature-controlled and can destroy insulin
- Split your supplies. Keep insulin and essentials in both carry-on and checked luggage in case of loss
- Take specialist travel insurance. An EHIC alone does not cover all emergencies or repatriation
- Know your climate risks. Heat speeds insulin absorption; cold slows it and increases hypo risk
- Monitor blood glucose more often abroad. Travel, time zones, unfamiliar food, and climate change can all affect your levels
- Never stop taking insulin if you’re unwell. Continue insulin even if you cannot eat solid foods; focus on carbohydrate drinks instead
- Carry a diabetes identity card. In an emergency, medical staff need to know you have diabetes immediately
Questions to Ask Your GP Before You Travel
Write these questions down and ask during your pre-travel appointment:
- “Do you recommend any changes to my insulin doses for my destination (time zone, climate, activity level)?”
- “What is the generic (chemical) name of my insulin, in case I need it abroad?”
- “Can you provide a letter for airport security confirming I need to carry syringes and insulin?”
- “Should I carry a glucagon emergency kit, and do I know how to use it?”
- “What are the signs of diabetic ketoacidosis (DKA), and when should I seek emergency care?”
- “Are there any activities or sports I should avoid during my trip?”
Frequently Asked Questions
Can I take insulin on a plane?
Yes. Insulin and diabetic supplies are exempt from the 100ml liquid rule on UK flights. Always carry insulin in your hand luggage in its original pharmacy packaging, and never check it into the hold – the hold can drop below freezing on long-haul flights, which damages insulin.
Do I need a doctor’s letter to travel with insulin and needles?
Yes. Ask your GP for a printed letter confirming your diagnosis, the medications and devices you carry, and the medical necessity of needles and lancets. Some destinations – including the UAE, Singapore, and parts of South-East Asia – require this letter at customs. Carry it with your passport, not packed.
How do I store insulin while travelling abroad?
Insulin must be kept cool but not frozen. Use an insulated travel pouch with a cool pack for the journey. Once at your accommodation, store insulin in a fridge between 2 and 8 degrees Celsius. Pre-loaded pens you are using day-to-day can be kept at room temperature for up to 28 days. Avoid leaving any insulin in direct sunlight or in a hot car.
How should I adjust my insulin doses across time zones?
Speak to your diabetes team or GP at least four weeks before travel – never guess. The general principle: if you fly east and lose hours, your day is shorter and you may skip a basal dose; if you fly west and gain hours, you may need an extra dose. Get a written protocol you can follow alongside finger-stick glucose monitoring.
What should I do if I have a hypo while abroad?
Treat it the same way as at home – 15 to 20g of fast-acting glucose (such as 4-5 jelly babies, 150ml of full-sugar cola, or a glucose gel), wait 15 minutes, then re-test. Carry hypo treatment everywhere you go. If symptoms do not improve or you become unable to swallow, ask someone to call the local emergency number (112 across most of Europe).
Will my GHIC cover diabetes treatment in the EU?
Yes – the GHIC entitles you to medically necessary state healthcare for chronic conditions including diabetes while you are visiting the EU, EEA, and Switzerland, at the same cost a local resident would pay. It does not cover repatriation, private clinics, or insulin supplies bought outside hospital. Always pair the GHIC with proper travel insurance.
Useful Resources and Sources
The following organisations provide detailed, evidence-based guidance on travelling with diabetes:
- Diabetes UK – Travel Guide – Comprehensive advice from the UK’s leading diabetes charity, including country-specific tips and insurance guidance
- EHIC.org.uk – Apply for Your European Health Insurance Card – Official government site to apply for an EHIC if you’re travelling to an EU member country
- NHS.uk – Diabetes and Exercise – NHS guidance on managing diabetes during activity and travel
- Fit for Travel – NHS Travel Health Service – NHS resource for vaccinations, health risks, and medical care in specific countries
Summary: Confident Travel with Diabetes
Travelling with diabetes is safe and enjoyable when you plan ahead. The steps are straightforward: see your GP, arrange insurance, pack carefully, split your supplies, and monitor your blood glucose more often. With these precautions in place, you can travel with confidence.
Whether you’re heading to a warm beach, a cold ski resort, or a bustling city, the same principles apply. Be prepared, stay aware, and don’t hesitate to seek medical help if needed. Your diabetes is manageable, and your holiday deserves to be.
Ready to explore more about managing your health while away? and offer additional information for specific travel situations.
Disclaimer: This article is for information only and does not constitute medical advice. Always consult your GP or a qualified healthcare professional before travelling if you have diabetes. Your doctor can provide personalised advice based on your specific medication, travel destination, and health history. In emergencies abroad, seek immediate medical attention from a local healthcare provider.
Join the community
For more practical health advice for over-50s living with diabetes, join our Facebook community where we share weekly tips, NHS updates, and reader stories.









