Overactive Thyroid Symptoms: What You Need to Know and When to See Your GP
An overactive thyroid, or hyperthyroidism, affects around 1 in 50 women and is 6 to 10 times more common in women than men. If you’re over 50, you may notice changes in how you feel – sudden weight loss, racing heartbeat, or persistent anxiety – that catch you off guard. This guide explains what overactive thyroid symptoms feel like, what causes them, and your options for treatment on the NHS or privately.

What Exactly Is an Overactive Thyroid?
Your thyroid is a small gland in your neck that produces hormones. These hormones control how fast your body works – your metabolism, heart rate, temperature, and energy levels. When your thyroid produces too much hormone, everything speeds up.
An overactive thyroid means your body is running too fast. Your heart pumps quicker, your metabolism burns calories faster, and your nervous system becomes over-stimulated. This condition is called hyperthyroidism.
In the UK, overactive thyroid affects about 1 in 100 people. It is significantly more common in women, particularly after age 50. If your mother or grandmother had thyroid problems, your risk is higher.
Watch: The Treatment Paradox – Understanding Hyperthyroidism
An overactive thyroid can cause symptoms that seem contradictory – losing weight while feeling exhausted, or feeling anxious despite doing nothing stressful. This cinematic overview unpacks the condition, explains how diagnosis works, and compares NHS and private treatment options in the UK.
Overactive Thyroid Symptoms: How They Develop
Overactive thyroid symptoms can appear suddenly or develop slowly over weeks. You may not recognise them at first because they overlap with stress, menopause, or ageing. Here are the most common signs:

Common symptoms of hyperthyroidism (overactive thyroid) to watch for
Physical Symptoms You Might Notice
- Unintended weight loss despite normal or increased appetite
- Rapid or irregular heartbeat (palpitations or fluttering)
- Trembling hands or shakiness
- Excessive sweating or heat intolerance
- Tiredness and muscle weakness, even after rest
- Swelling in your neck (goitre) from an enlarged thyroid
- Frequent bowel movements or diarrhoea
- Brittle or thinning hair
Emotional and Mental Symptoms
- Nervousness, anxiety, or panic attacks without obvious cause
- Irritability or mood swings
- Difficulty concentrating or brain fog
- Sleep problems or insomnia despite feeling exhausted
If you spot several of these symptoms, a GP appointment is the right step. Many people assume these changes are just part of getting older, but they deserve proper investigation.
What Causes an Overactive Thyroid?
Understanding the cause helps explain why treatment differs from person to person.
Graves’ Disease (Most Common)
About 4 in every 5 people with overactive thyroid have Graves’ disease. This is an autoimmune condition where your immune system mistakenly attacks your thyroid gland. Graves’ disease is hereditary and more common in women.
Thyroid Nodules
Sometimes extra lumps (nodules) form inside your thyroid gland. These nodules can produce thyroid hormone independently. A single overactive nodule is called toxic adenoma. Multiple nodules cause toxic multinodular goitre. This is more common as you age.
Medications and Other Causes
Certain medicines can trigger overactive thyroid. Amiodarone, used to treat irregular heart rhythms, is the most common culprit. Too much iodine from supplements or contrast dye can also trigger symptoms.
How Is an Overactive Thyroid Diagnosed?
If your GP suspects overactive thyroid, they will arrange a blood test. This measures TSH (thyroid-stimulating hormone) and T4 (thyroxine). Your TSH is usually low when your thyroid is overactive, and your T4 is elevated.
A blood test can be done at your GP surgery. Results usually take 1-2 weeks. If your results confirm overactive thyroid, your GP will refer you to an endocrinologist. An endocrinologist is a specialist in hormone conditions. They will arrange further tests to identify the cause.
Your endocrinologist may also arrange a thyroid ultrasound or a radioiodine scan. These tests help guide your treatment plan.
NHS vs Private Treatment: Costs and Waiting Times
Both NHS and private care can effectively treat overactive thyroid symptoms. The choice often depends on how quickly you need results.
NHS Treatment
On the NHS, treatment is completely free. Your GP refers you to an endocrinologist at your local NHS hospital. As of March 2026, routine endocrinology appointments have an average waiting time of 10-13 weeks [VERIFY]. Urgent referrals may be seen within 2-3 weeks.
NHS treatment follows NICE guideline NG145 for thyroid disease management. Treatment options include:
- Antithyroid drugs – typically carbimazole, taken daily for 12-18 months
- Radioiodine therapy – a one-off treatment that destroys overactive thyroid cells
- Surgery – removing part or all of your thyroid (thyroidectomy)
Private Treatment
Private treatment is faster. You can usually see a private endocrinologist within 1-2 weeks.
Private consultant costs in the UK (2026):
- Initial consultation: £135-£300 depending on clinic and location [VERIFY]
- Thyroid ultrasound: £100-£200
- Blood tests: £80-£150
- Radioiodine therapy: £2,500-£5,000 [VERIFY]
- Thyroid surgery: £8,000-£15,000 [VERIFY]
Private insurance (Bupa, AXA Health, Vitality) may cover some or all of these costs. Check your policy first.
For a broader look at how NHS and private costs compare across common procedures, see our guide to the 10 most common surgeries for over-50s.
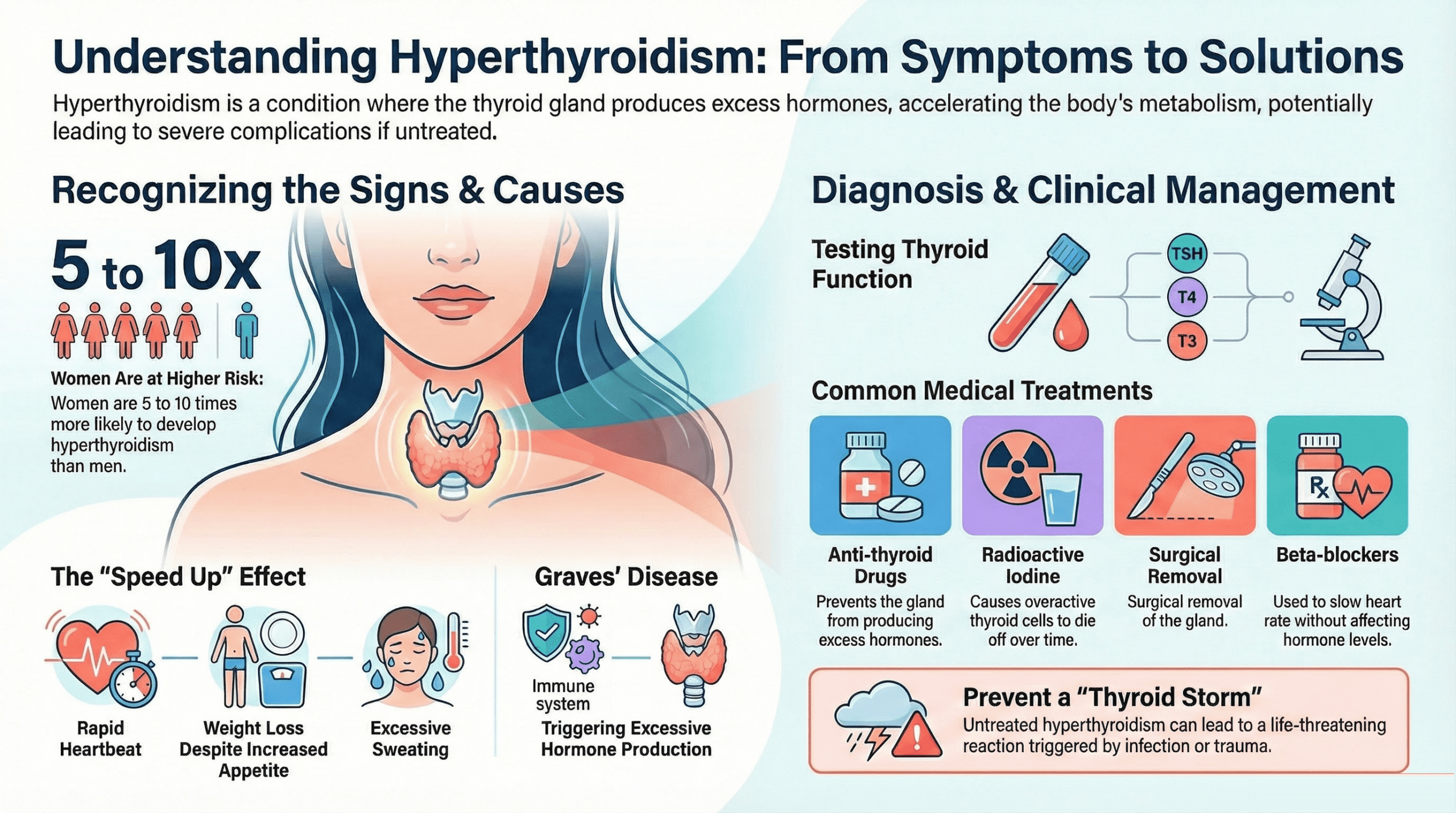
Treatment Options Explained
Antithyroid Drugs
This is usually the first-line treatment for Graves’ disease. Carbimazole blocks your thyroid from producing excess hormone. You take it daily, and levels return to normal over 4-6 weeks. Most people take carbimazole for 12-18 months. About 50% go into remission; the other 50% need further treatment.
Radioiodine Therapy
You swallow a capsule of radioactive iodine that destroys overactive thyroid cells over 6-12 weeks. Most people eventually develop an underactive thyroid afterwards. This requires lifelong levothyroxine, which is straightforward to manage.
If your treatment leads to an underactive thyroid, our guide to hypothyroidism and underactive thyroid explains what to expect and how it is managed.
Surgery
A surgeon removes part or all of your thyroid under general anaesthetic. Recovery takes 1-2 weeks for normal activities. Like radioiodine, surgery often results in hypothyroidism.
Frequently Asked Questions About Overactive Thyroid
What are the most common symptoms of an overactive thyroid?
The most common symptoms include unexplained weight loss, a rapid or irregular heartbeat, anxiety and irritability, trembling hands, increased sweating, difficulty sleeping, fatigue, and frequent bowel movements. Women may notice lighter or irregular periods. Symptoms often develop gradually, which is why many people – particularly those over 50 – attribute them to stress or ageing before seeking a diagnosis.
How is an overactive thyroid diagnosed?
Diagnosis starts with a simple blood test measuring thyroid-stimulating hormone (TSH) and thyroid hormones (T3 and T4). If TSH is low and T3 or T4 are high, this confirms hyperthyroidism. Your GP may then arrange additional tests such as thyroid antibody tests (to check for Graves’ disease) or a thyroid ultrasound. The blood test is quick, reliable, and available through your GP surgery.
Can an overactive thyroid be cured?
In many cases, yes. Treatment options include antithyroid medication (such as carbimazole), which controls the condition and sometimes leads to long-term remission. Radioactive iodine treatment is a common permanent solution that gradually reduces thyroid activity. Thyroid surgery (thyroidectomy) is used in more complex cases. After radioactive iodine or surgery, you will likely need daily thyroid hormone replacement tablets for life.
Is an overactive thyroid serious?
If left untreated, an overactive thyroid can lead to serious complications including heart problems (atrial fibrillation, heart failure), bone thinning (osteoporosis), and in rare cases a life-threatening condition called thyroid storm. However, with proper treatment, most people manage the condition effectively and live normal, healthy lives. Early diagnosis and treatment are important to prevent complications.
Can stress cause an overactive thyroid?
Stress does not directly cause an overactive thyroid, but it may trigger or worsen autoimmune conditions like Graves’ disease (the most common cause of hyperthyroidism) in people who are genetically predisposed. Severe emotional or physical stress can sometimes precede the onset of Graves’ disease. Managing stress through exercise, relaxation techniques, and adequate sleep supports overall thyroid health.
Can I develop overactive thyroid after age 50?
Yes. Thyroid nodules become increasingly common with age, and Graves’ disease can develop or worsen during menopause.
What is the difference between overactive and underactive thyroid?
Overactive means too much hormone – your metabolism speeds up. Underactive means too little – your metabolism slows. A simple blood test distinguishes between them.
Will I need medication for life?
It depends on the cause and treatment. About 50% of people on antithyroid drugs achieve remission. Radioiodine and surgery are permanent fixes but often require lifelong thyroid hormone replacement.
Is overactive thyroid hereditary?
Graves’ disease has a strong genetic component. If a close relative has it, your risk is elevated. However, not everyone with a family history develops it.
What Should You Ask Your GP?
- Will you arrange a blood test to check my thyroid function?
- How long will the results take?
- If results are abnormal, will I be referred to an endocrinologist?
- What is the typical waiting time for a specialist in my area?
- Could any of my current medicines be causing thyroid symptoms?
Key Takeaways
- Overactive thyroid symptoms include unexplained weight loss, racing heartbeat, nervousness, sweating, and persistent tiredness.
- Graves’ disease causes about 80% of cases. Thyroid nodules and certain medications are other common causes.
- A simple blood test confirms diagnosis. NHS tests are free; results take 1-2 weeks.
- NHS treatment is free but involves waiting 10-13 weeks for a specialist. Private consultations cost £135-£300 with appointments available within 1-2 weeks.
- Treatment options include antithyroid drugs, radioiodine therapy, or surgery – most people live normal, healthy lives once treated.
- Early diagnosis prevents serious complications including heart problems and osteoporosis.
Next Steps
If you recognise overactive thyroid symptoms in yourself, book a GP appointment. A simple blood test can confirm whether your thyroid is the problem.
For further reading, visit the NHS.uk overactive thyroid page or Thyroid UK for support and information.
Our guide to private scan costs in the UK covers thyroid ultrasound and other diagnostic imaging prices.
This article is for information only. Always consult your GP or a qualified healthcare professional before making health decisions.









