Travel Health Checklist for Over 50s: Your Pre-Trip Guide
Whether you are planning a relaxing week in the Mediterranean or a long-haul adventure further afield, a little preparation protects your health – and your holiday. After 50, small details like medication timing, vaccinations, and insurance cover matter more. Age UK reports that around 60 per cent of over-60s travel with at least one chronic health condition, yet many still set off without adequate preparation. This comprehensive travel health checklist walks you through everything to sort out before departure, so you can travel with confidence and enjoy every moment of your trip.

We have built this guide around the core essentials that make the biggest difference to how your holiday goes – from vaccinations and medication to insurance, DVT prevention, sun safety, jet lag, and what to pack. Each section includes practical actions, and the printable checklist at the end pulls everything into a single ready-to-use format.
See Your GP 6 to 8 Weeks Before You Travel
Your GP is the best starting point for any trip abroad. Book an appointment six to eight weeks before departure, especially if you have an ongoing condition such as diabetes, heart disease, arthritis, or COPD. Your GP can check that your destination is suitable, review your medication, arrange any vaccinations you need, and confirm that you are medically fit to fly – particularly important if you have had a recent heart event, stroke, or surgery.
Ask for a printed medical summary that lists your diagnoses, current medications (with generic names, doses, and timing), known allergies, and emergency contact details. This summary is invaluable if you need treatment abroad, particularly where there is a language barrier.
If your GP surgery does not offer every vaccination you need, they can refer you to a travel clinic. NHS travel services are free but often have 2-3 week waits; private travel clinics such as Boots Travel Health or Trailfinders typically offer appointments within days at around £20-£50 per vaccine.
Watch: The 2026 Travel Health Checklist for Over-50s
In this short cinematic guide, you’ll see exactly what to organise before your next holiday – from the GP appointment to book six to eight weeks ahead, to packing medications, choosing travel insurance with pre-existing condition cover, and applying for a free GHIC card for European healthcare.
Travel Vaccinations and Destination Health Advice
Vaccination requirements change regularly and depend entirely on where you are travelling. The UK government-backed TravelHealthPro (NaTHNaC) website lists up-to-date country-by-country advice on recommended vaccinations, malaria risk, and local disease outbreaks. NHS Fit for Travel provides equivalent NHS-verified information.
The most common vaccinations for over-50s travelling outside the UK are summarised below, with typical timing requirements:
| Vaccination | Typical destinations | Timing before travel |
|---|---|---|
| Polio booster (IPV) | Most destinations outside UK | 1 dose at least 4 weeks before |
| Typhoid | Asia, Africa, Central America | 1 dose at least 2 weeks before |
| Hepatitis A | Destinations with poor sanitation | 1 dose at least 2 weeks before |
| Yellow fever | Sub-Saharan Africa, South America | 1 dose at least 10 days before |
| Malaria tablets | Parts of Africa and Asia | Start 1-2 days before; continue during and 4 weeks after |
| COVID-19 booster | Check destination entry rules | At least 2 weeks before if required |
Some vaccinations require multiple doses spread over several weeks, so do not leave this to the last minute. Certain destinations also require proof of vaccination (such as yellow fever) before they permit entry.
Pack Your Medicines Properly
Carry at least double your usual medication supply in your hand luggage, not the hold. Ask your GP for a “To Take Out” (TTO) prescription – enough to cover your entire trip plus two or three extra days in case of delays.
- Keep medicines in the original labelled pharmacy container. Customs officers may refuse unmarked tablets.
- Carry a letter from your GP or pharmacist confirming each medication is prescribed to you and its medical necessity.
- Check legality at your destination. Some UK-prescribed medicines – including certain painkillers and controlled drugs – are banned or restricted in other countries. GOV.UK and your destination’s embassy website will confirm.
- Plan for temperature-sensitive medicines. Insulin, some biologics, and certain liquid antibiotics need cool storage. Use an insulated travel pouch, and ask your accommodation in advance whether a fridge is available.
Our guide on travelling with diabetes covers insulin storage, airport security, and dose adjustments in detail.
Manage Medication Timing Across Time Zones
Crossing several time zones complicates regular medication timing – particularly for medicines you take once or twice a day. General rules:
- Flying east (losing hours): Your day is shorter. After you arrive, take your medication at the new local time. You may skip one dose, depending on the drug – your GP will confirm.
- Flying west (gaining hours): Your day is longer. Keep to your original dose schedule for as long as possible, or take an extra dose if advised. Again, check with your GP in advance.
- For critical medications (insulin, anticoagulants, anti-arrhythmics, heart failure drugs), never guess. Get a written protocol from your GP or pharmacist before you leave.
Set phone alarms for every dose. Carry your medication letter, and keep insulin and other essential medicines in your hand luggage – lost checked baggage means lost treatment.
Travel Insurance With Pre-Existing Conditions
Travel insurance is non-negotiable once you are over 50, particularly if you have any pre-existing conditions. Standard mainstream policies often exclude declared conditions or charge significant premiums; specialist over-50s providers are usually more comprehensive and competitive. Always declare every condition, even well-controlled ones – non-disclosure invalidates your entire policy and leaves you personally liable for all medical costs abroad.
When comparing policies, look for these minimum cover levels:
- Medical cover and repatriation: At least £10 million. Air ambulance evacuation alone can cost £10,000-£100,000.
- Trip cancellation: £5,000-£10,000 is a sensible floor, particularly if your condition could flare before departure.
- Pre-existing condition cover: Declared and priced in – expect a 10 to 50 per cent loading on the base premium, or a flat surcharge of £30-£50 per condition.
- Winter sports add-on: Needed if you plan to ski, snowboard, or mountain walk.
Options include specialist over-50s providers (AllClear, Staysure, Free Spirit, Age UK), mainstream travel insurers (Post Office, Sainsbury’s, Boots), and independent review sites such as Which?, which flag unexpected exclusions. If you travel more than twice a year, an annual multi-trip policy is usually cheaper than single-trip cover.
Our complete guide to travel insurance with medical conditions compares specialist UK providers, typical premiums for common conditions, and what to check in the small print.
GHIC for EU and EEA Healthcare
The UK Global Health Insurance Card (GHIC) replaced the EHIC in December 2021. It gives UK residents access to state-provided healthcare in the EU, Iceland, Liechtenstein, Norway, and Switzerland at the same cost a local resident would pay – often free or heavily subsidised.
What GHIC covers:
- Medically necessary state healthcare while you are in the country
- Treatment of chronic and pre-existing conditions that becomes necessary during your visit
- Routine maternity care (but not intentional travel to give birth)
What GHIC does not cover:
- Private treatment, private hospitals, or private clinics
- Repatriation flights home if you become seriously ill
- Medical evacuation or air ambulance
- Countries outside the EU, EEA, and Switzerland (USA, Thailand, Australia, etc.)
- Trip cancellation, lost baggage, or other non-medical claims
Check your GHIC expiry date at least 12 weeks before travel. Renewal is free and takes 1-2 weeks through the NHS GHIC application page. GHIC is not a substitute for travel insurance – the two work together, and you need both.
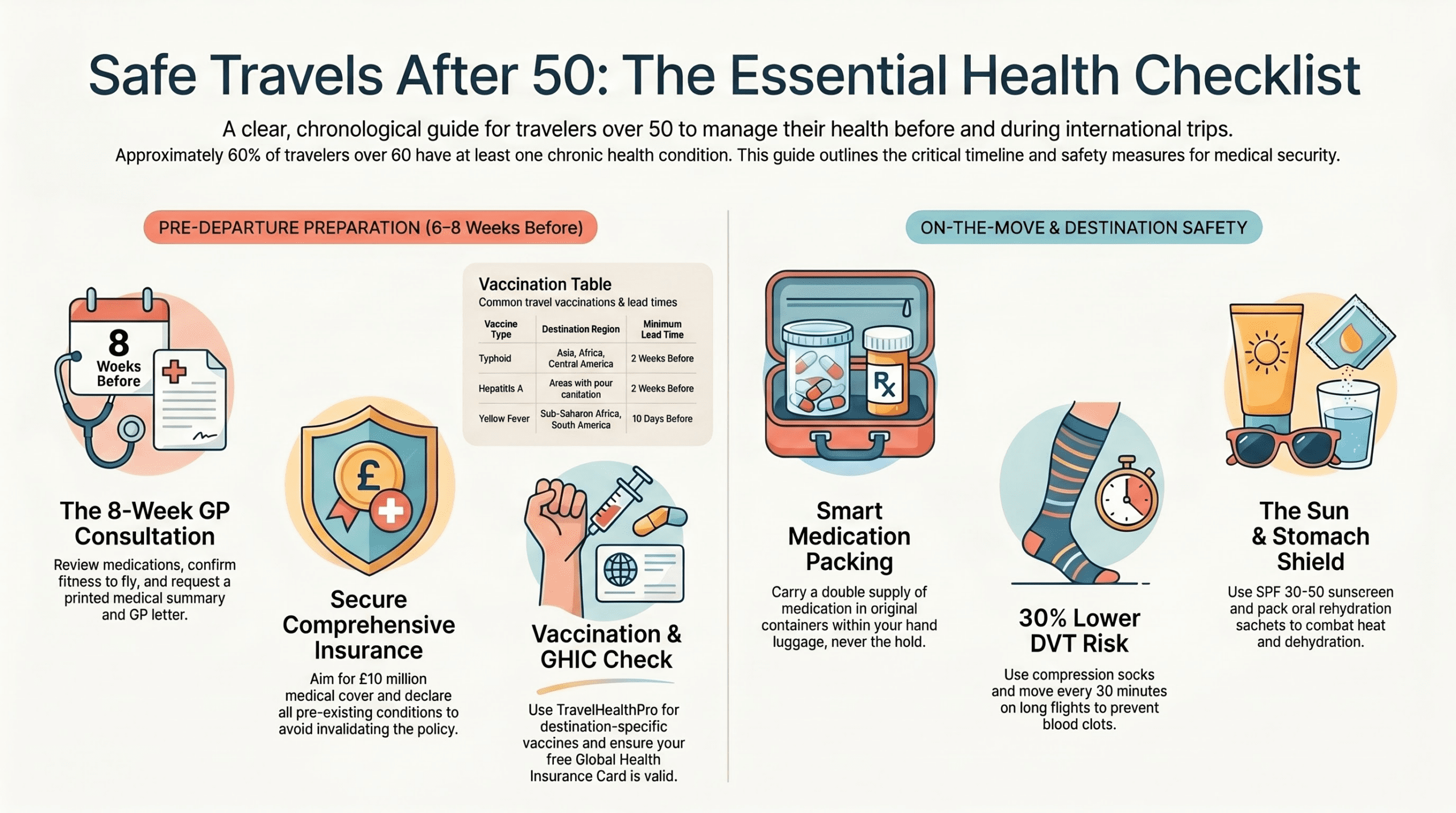
Prevent Deep Vein Thrombosis on Long Flights
Sitting still for long periods raises your risk of deep vein thrombosis (DVT), and that risk climbs sharply after 50. NHS research suggests good use of compression socks on long flights reduces clot risk by around 30 per cent. Four simple steps make a real difference:
- Wear flight compression socks that come to just below the knee, from about two hours before departure until roughly 24 hours after arrival. They cost £20-£40 a pair from most chemists.
- Move every 30 minutes – stand up, walk the aisle, or do calf raises and ankle rotations in your seat.
- Stay hydrated with around 250ml of water each hour, and avoid excessive alcohol and caffeine, both of which thicken blood.
- Keep blood flow unrestricted – avoid tight seatbelts across the thighs, rolled-up trouser legs, or crossed legs for long stretches.
If you have had a previous DVT, major recent surgery, or take certain medications, ask your GP whether you need additional prevention such as an injectable low-molecular-weight heparin dose before flying. These must be prescribed and carried in hand luggage with your GP letter.
Protect Yourself From Sun and Heat
Older skin is more sensitive to the sun, and sunburn in a hot climate is more than a nuisance – it dehydrates you, raises your risk of skin cancer, and can tip you into heat exhaustion. Choose a broad-spectrum sunscreen of at least SPF 30 (SPF 50+ in strong sun) with four or five-star UVA protection. Apply it 20 minutes before going outside, and reapply every two hours or after swimming.

Stay out of direct sun between 11am and 3pm, wear a wide-brimmed hat, and use UV-blocking sunglasses. Drink at least 2-3 litres of water daily in hot weather – more if you are active. Our guide to the 10 most common sunscreen mistakes explains what most people get wrong.
Watch for the warning signs of heat exhaustion: dizziness, nausea, headache, rapid heartbeat, heavy sweating, and intense thirst. Move to shade or air conditioning, drink cool water slowly, and apply cool damp cloths to the skin. If symptoms do not improve within 30 minutes, or if the person becomes confused or stops sweating, call for emergency help – heatstroke is a medical emergency.
Stay Safe With Food, Water, and Stomach Upsets
Traveller’s diarrhoea is the most common holiday illness, and it hits over-50s harder because dehydration happens faster. Pack oral rehydration sachets (Dioralyte or similar) in your suitcase, an anti-diarrhoeal such as loperamide (Imodium), and a general anti-sickness tablet.
In higher-risk destinations, stick to bottled or purified water for drinking and teeth brushing, avoid ice in drinks, and choose hot, freshly cooked food over salads or buffet items that have been standing. Peel fruit yourself, and avoid unpasteurised dairy. A 60ml bottle of 70 per cent alcohol hand sanitiser is worth its weight in gold – use it before eating and after public transport.
Build a Sensible First Aid Kit
A small first-aid kit saves many a holiday. Core items:
- Paracetamol (500mg) and ibuprofen (200mg) for pain, fever, or headache
- Loperamide (Imodium) and oral rehydration sachets (Dioralyte)
- Antihistamine tablets (cetirizine or loratadine) for bites, stings, or hay fever
- Antiseptic wipes, plasters, and waterproof wound dressings
- Hydrocortisone cream for bites, rashes, or insect reactions
- Antiseptic ointment (such as Savlon) for cuts and grazes
- A digital thermometer and small tweezers
Our essential first aid kit for travelling safely goes through every item in detail, including insect repellent and additions for specific conditions.
Prepare for Insect Bites and Stings
Mosquitoes, ticks, and biting flies are more than irritating – in some destinations they spread serious illness including malaria, dengue fever, and Lyme disease. Use a DEET-based repellent (30-50 per cent) on exposed skin, cover up at dusk, and sleep under a permethrin-treated mosquito net in high-risk areas. Pack a small tube of antihistamine cream for bites you do pick up. Severe reactions – swelling of the face, difficulty breathing, or a rapidly spreading rash – are a medical emergency.
Manage Jet Lag and Sleep Disruption
Crossing several time zones disrupts sleep and medication timing. A few simple steps help your body reset faster:
- Shift your sleep schedule 2-3 days before travel – going to bed earlier for eastbound flights and later for westbound.
- Get natural light at your destination, especially early morning. Daylight is the strongest signal to your body clock.
- Avoid heavy meals and alcohol near bedtime, and limit afternoon caffeine.
- Stay active during the day – even a short walk helps your body recognise the new time.
- If needed, consider melatonin 0.5-2mg taken 30 minutes before your desired bedtime, but ask your GP first, particularly if you take sleeping tablets or antidepressants.
Know Your Destination’s Healthcare System
Research how emergency healthcare works where you are going, and save the local emergency number in your phone. In most of Europe it is 112; other countries vary. Save your insurer’s 24/7 helpline, your accommodation address, the nearest hospital, and the UK embassy contact details before you fly.
If you do fall ill or get injured abroad, contact your insurer’s emergency line as soon as possible. Our practical guide on what steps to take if you are injured on holiday walks through exactly what to do, what paperwork to keep, and how to make a successful claim.
Your Printable Pre-Travel Checklist
Use this checklist four to six weeks before departure:
| Category | Task | When | Done |
|---|---|---|---|
| BEFORE YOU GO (6+ weeks ahead) | |||
| Documents | Check GHIC expiry and renew if needed | 12 weeks before | [ ] |
| GP visit | Book pre-travel appointment | 6-8 weeks before | [ ] |
| Vaccinations | Receive any vaccinations advised | 4-10 weeks before | [ ] |
| Medications | Request TTO prescription and GP letter | 2-4 weeks before | [ ] |
| Insurance | Buy travel insurance and declare all conditions | 2-4 weeks before | [ ] |
| Planning | Note nearest hospital, embassy, insurer helpline | 2-3 weeks before | [ ] |
| PACKING | |||
| Hand luggage | All medications, GP letter, GHIC, insurance details, prescription copies | Day of travel | [ ] |
| First aid kit | Paracetamol, ibuprofen, antihistamine, loperamide, plasters, antiseptic, thermometer | Day before travel | [ ] |
| Sun and heat | SPF 30-50+ sunscreen, wide-brimmed hat, sunglasses, after-sun | Day before travel | [ ] |
| DVT prevention | Compression socks (flights 4+ hours), water bottle, movement alarm | Day before travel | [ ] |
| AT YOUR DESTINATION | |||
| Medication timing | Adjust to local time; set phone alarms | Daily | [ ] |
| Hydration | 2-3 litres of water daily, limit alcohol | Daily | [ ] |
| Sun safety | Reapply sunscreen every 2 hours; avoid midday sun | Daily | [ ] |
| Food safety | Hot freshly cooked food; bottled water; no ice from tap | Daily | [ ] |
| Movement | Stretch and walk regularly; wiggle toes on long sits | Daily | [ ] |
Key Takeaways
- Book a GP appointment 6-8 weeks before travel to check destination suitability, medications, vaccinations, and fitness to fly.
- Use TravelHealthPro and NHS Fit for Travel for up-to-date country-specific advice.
- Pack double your usual medication with a TTO prescription and GP letter, in original labelled containers, in hand luggage.
- For long-haul flights, plan medication timing across time zones in advance with your GP – never guess with critical drugs.
- Buy specialist travel insurance covering every declared condition. Minimum £10 million medical cover and £5,000+ cancellation cover.
- Apply or renew a free UK GHIC card for EU and EEA travel. It complements travel insurance but does not replace it.
- Prevent DVT on long flights with compression socks, hourly movement, and plenty of water.
- Use SPF 30-50+ broad-spectrum sunscreen, stay out of midday sun, and know the warning signs of heat exhaustion.
- Pack oral rehydration sachets, loperamide, antihistamines, and alcohol hand sanitiser for stomach upsets and bites.
- Manage jet lag with pre-travel schedule shifts, morning daylight at destination, and cautious use of melatonin if advised.
Frequently Asked Questions
How far in advance should I book my GP appointment before travelling?
The NHS recommends booking your pre-travel GP appointment six to eight weeks before you fly. This gives enough time for any vaccinations to take effect, for repeat prescriptions to be issued, and for your GP to write a medical letter if needed. Last-minute trips can still be supported, but some vaccinations need multiple doses and may not be fully effective.
What vaccinations do I need for travelling abroad?
Vaccination requirements depend entirely on your destination. Routine NHS boosters such as polio, tetanus and MMR should be up to date for any international travel. Specific destinations may require yellow fever, typhoid, hepatitis A, or COVID-19 boosters. Check the official UK government TravelHealthPro website or NHS Fit for Travel for country-by-country advice.
Do I still need travel insurance if I have a GHIC card?
Yes. The GHIC (Global Health Insurance Card) only covers state-provided medical care in the EU, EEA and Switzerland – and it does not pay for repatriation, private hospitals, or medical evacuation. You should always have comprehensive travel insurance alongside your GHIC, particularly if you have any pre-existing health conditions or are travelling outside Europe.
How can I reduce my risk of DVT on a long-haul flight?
NHS guidance suggests wearing flight compression socks rated for 14 to 17 mmHg from a couple of hours before take-off until around 24 hours after landing. Move every 30 minutes, do simple calf raises and ankle rotations, drink around 250ml of water per hour, and avoid excessive alcohol. If you have had a previous DVT or recent major surgery, ask your GP whether you need additional preventative measures before flying.
Can I take prescription medicines on a plane?
Yes. Always carry prescription medicines in your hand luggage, in their original labelled pharmacy packaging. Take a letter from your GP or pharmacist stating each medication is prescribed to you, particularly for controlled drugs and injectables. Some UK-prescribed medicines, including certain painkillers, are restricted abroad – check the destination country embassy website and Gov.uk before travelling.
How long does a GHIC card last and how do I renew it?
The UK Global Health Insurance Card (GHIC) is valid for five years. You can apply for or renew a GHIC for free directly through the official NHS GHIC application page on gov.uk – it usually arrives within two weeks. Avoid third-party sites that charge a fee. Check your expiry date at least 12 weeks before travel, as you cannot use an expired card while abroad.
Further Reading and Trusted Sources
For additional, evidence-based travel health advice, Age UK’s travel pages cover mobility support at airports and travel companion schemes, while the Foreign Office’s country-by-country travel advice is worth a final check in the week before you fly.
Join the community
For weekly travel health tips, NHS updates, and reader stories, join our Facebook community where over-50s share practical advice for staying well at home and abroad.
Disclaimer: This article is for information only and does not replace professional medical advice. Always consult your GP or a qualified healthcare professional before travelling with a health condition, and read your insurance policy documents carefully before purchase. Destination health guidance can change quickly; verify recommendations at NHS Fit for Travel or TravelHealthPro close to your departure date.









