A pacemaker-like microregulator has been developed which helps block the pain of inflamed joints such as those in people who suffer from rheumatoid arthritis. The tiny device is fitted under the skin near the collarbone and sends electrical pulses to a key nerve, the vagus nerve. When the electrical pulses reach the spleen, they trigger a decrease in the production of inflammatory causing proteins called cytokines.
Currently rheumatoid arthritis patients take a cocktail of drugs to dampen the immune system but these are prone to side-effects. Experts have found that by stimulating the vagus nerve, the beneficial effects are experienced without the harmful side effects.
The device is currently being tested in the Netherlands and scientists hope it will be available in the UK by 2020. The early results have been very promising with the majority of patients seeing an improvement in their disease symptoms. Bioelectronic devices such as these are also improving rapidly and could be used to treat a variety of conditions. Trials are already taking place in patients with Crohn’s disease. The devices themselves are being made smaller with all the necessary components included in one small micro regulator meaning no wires or batteries are needed.
The development has been welcomed in the UK and Clare Jacklin of the National Rheumatoid Arthritis Society said:
“This new device may well be impactful for some patients depending on their disease profile.”
While these early results are promising, it will take time for the devices to be approved for general use. But in the future, bioelectronic medicine could offer an alternative to drug treatments for many patients suffering from auto immune diseases.
What is rheumatoid arthritis?
Rheumatoid arthritis is an autoimmune disease that causes inflammation, mainly in your joints and the tissues around them. This causes stiffness, pain and swelling. It is the second most common type of arthritis in the UK after osteoarthritis. It affects one in every 100 people and is three times more prevalent in women than men. You’re most likely to develop rheumatoid arthritis between the ages of 40 and 60, although you can develop it at any age. Most often people develop the inflammation in their hands and feet but it can affect any joint, as well as other parts of your body.
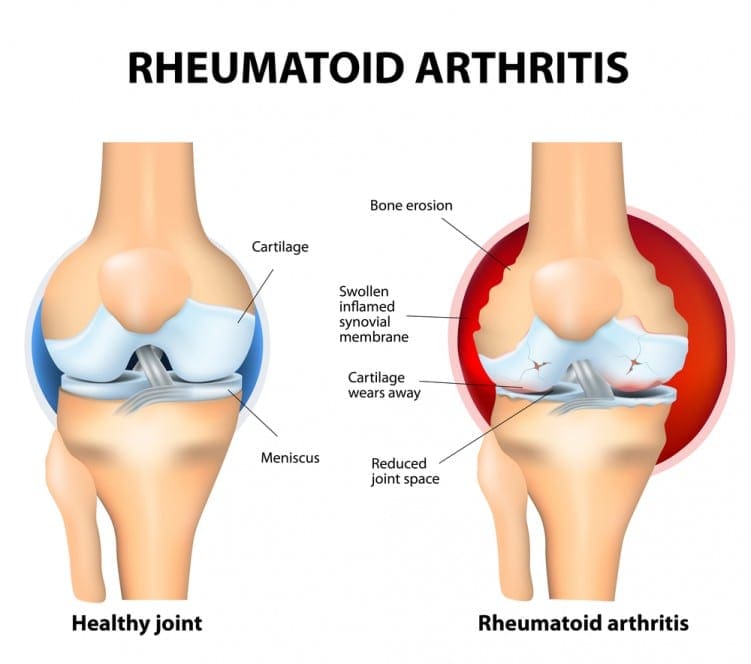
The immune system of a patient with rheumatoid arthritis attacks the lining of the joints, causing them to swell. As opposed to the wear and tear damage that occurs with osteoarthritis, rheumatoid arthritis affects the lining of the joints, resulting in painful swelling that can lead to bone erosion and joint deformity. Eventually the affected joints may become permanently damaged.
What are the symptoms?
Symptoms of rheumatoid arthritis tend to come and go and you may have flare-ups when your joints become more inflamed and painful. Common symptoms include:
- Pain and swelling around your joints, making them feel tender and warm
- Stiffness, especially in the morning or if you sit for a long time
- Flu-like symptoms such as a fever, feeling hot and sweating
- Tiredness making you feel depressed and irritable
- Weight loss
- Inflammation in the eyes
- Anaemia or a lack of red blood cells
You may also find our guide to hi-tech labour saving devices – blessing or burden? helpful.
What causes rheumatoid arthritis?
The smooth lining of the membranes that surround our joints is called the synovium. This produces a clear fluid, synovial fluid, which lubricates and nourishes the cartilage and bones inside the joint capsule. When the immune system attacks the synovium, rheumatoid arthritis may occur.
The exact reasons why this happens are not fully understood. If other members of your family have the condition, you are more likely to get it. Your lifestyle may also increase your risk of developing the condition. If you smoke, you may be more likely to develop it. Other triggers include stress, infection and hormone changes.
How is it diagnosed?
In its early stages rheumatoid arthritis may be difficult to diagnose. Its signs and symptoms are similar to several other conditions. But it is important to be diagnosed as soon as possible because the sooner you start the treatment, the better it’s likely to work.
Your doctor will carry out a physical examination to check if there is any swelling around the joints. They should also ask you about your other symptoms and your medical and family history. They will arrange for you to have a blood test to check for a number of things, such as rheumatoid factor and anti-CCP antibodies. These are produced by a reaction in your immune system. Your doctor may also arrange for you to have an x-ray to look for changes in your joints.
What treatments are available currently?
Although there is no cure, a variety of treatments are available to slow down the disease and keep joint damage to a minimum. There are three main aspects to the treatment:
- drugs
- physical therapies
- surgery
What drugs may be prescribed?
- Painkillers and anti-inflammatory medicines such as ibuprofen
- Steroids
- Disease-modifying antirheumatic drugs (DMARDs)
- Biological medicines
What physical therapies may help?
A physiotherapist can give you exercises to help you stay flexible and build up your muscle strength. If you have problems with your hands, a hand specialist will help you with strategies to manage your pain and keep your hands functioning. They can advise you on aids available to help with everyday tasks. A podiatrist will advise you if you have problems with your feet and will help you find the right footwear to manage your condition. Hydrotherapy, where exercises are done in a special warm water pool, may also ease joint pain.
Many people with rheumatoid arthritis use complementary therapies to ease their symptoms. Acupuncture, aromatherapy and massage may relieve pain and stiffness and make you feel more relaxed. There is some evidence that omega-3 oils can help to ease joint pain and stiffness.
What about surgery?
If other treatments haven’t worked, you may be offered surgery. Operations vary from minor procedures to remove the inflamed lining of a joint, to more major surgery to replace a joint. Your doctor will advise you about the possible options.
What can I do to make my condition easier to live with?
- Strike a good balance between exercise and rest
- Find an exercise you enjoy and do it when you’re in the least amount of pain
- Eat a balanced diet and try to keep to a healthy weight
- Try to get a good night’s sleep to help with fatigue
- Don’t be afraid to talk about your condition and seek the help that is available
- Contact local support groups and talk to others living with the condition
- If you smoke, try cutting down or stopping completely
- Protect your joints from unnecessary strain
- Use labour saving gadgets and aids specially designed for people with arthritis
- Rearrange the rooms in your house to make sure things you use most are easy to reach
- Plan ahead and pace your day
An interesting study suggests that a green tea compound may help in the treatment of rheumatoid arthritis.
Finally, the unpredictability of your condition is frustrating and so it is vital to plan ahead and pace yourself. Make it clear to your family and friends that you have good days and bad and don’t be embarrassed to talk about this. Managing how you feel is as important as managing your symptoms. Try to talk to other people who suffer from the condition and try to become better informed to help you stay positive.
If you would like more information and advice, the following link will take you to the website of the National Rheumatoid Arthritis Society:
If you know someone who may benefit from this information, please Share it with them via the links at the bottom of this page.
For updates on arthritis and other topics concerning over 50s health, don’t hesitate to follow us on Facebook or sign up to our free newsletter The Best of Friends.








