Sciatica Treatment for Over-50s: Causes, Symptoms and Recovery in 2026
Sciatica affects millions of people in the UK, and for adults over 50, the pain can be severe and frustrating. You feel a sharp, burning sensation down one leg. Sitting makes it worse. Walking becomes difficult. But here’s the good news: with the right diagnosis and treatment, most people recover within weeks or months. This guide explains what sciatica really is, why you’re experiencing it, and what treatment options-both through the NHS and privately-can help you get relief.

We’ll also compare NHS waiting times and costs with private providers, so you can make an informed decision about your care in 2026.
Key Takeaways
- Sciatica is a symptom, not a diagnosis-it’s caused by irritation or compression of the sciatic nerve, often from a herniated disc, spinal stenosis, or degenerative disc disease.
- Common symptoms include sharp, burning leg pain, numbness, weakness, and tingling, usually on one side of the body.
- Over-50s are at higher risk due to disc deterioration, spinal stenosis, and degenerative changes.
- NHS treatment begins with your GP and typically includes physio, NSAIDs, and sometimes steroid injections-waiting times range from 6-12 weeks, cost-free at the point of care.
- Private physio costs £40-£80 per session; private surgery costs £8,000-£15,000 .
- Most people recover without surgery-relief often comes from physiotherapy, exercise, and time.
What Is Sciatica? Understanding Your Sciatic Nerve
Sciatica is not a medical diagnosis-it’s a symptom. For broader practical advice on protecting your spine day-to-day, see our companion guide on effective tips for preventing back pain. The term describes pain caused by irritation or compression of the sciatic nerve, the longest nerve in your body.
The sciatic nerve begins in your pelvis, travels through your buttocks, and runs down your legs to your feet. When something compresses or irritates this nerve anywhere along its path, you feel pain. That pain is sciatica.
The key insight for treatment: your pain is a symptom of an underlying cause. Finding and treating that cause-whether it’s a herniated disc, spinal stenosis, or degenerative changes-is what actually resolves your sciatica. Simply masking the pain with painkillers won’t fix the root problem.
This is why your GP will ask detailed questions about your pain, examine your back, and may order imaging scans. They’re looking for the cause, not just the symptom.
Sciatica Symptoms: What to Recognise
Sciatica symptoms vary in location, intensity, and how they affect you. Most people experience pain on one side of the body only.
Common signs include:
- Constant pain in one buttock or leg (rarely both sides)
- Sharp, burning, or searing pain (rather than a dull ache)
- Pain that worsens when sitting, bending forward, or lying down
- Numbness or weakness in the leg or foot
- Tingling or “pins and needles” sensation in the feet and toes
- Difficulty standing up, walking, or bearing weight on the affected leg
Pain intensity ranges from mild and occasional to severe and constant. Most people describe sciatica as more painful than lower back pain alone-because the nerve pain radiates and creates burning, electrical sensations.
The good news: it is rare for sciatica to cause permanent nerve damage. With appropriate treatment, inflammation usually subsides within a few weeks to a few months.
What Causes Sciatica? Over-50s Risk Factors
Adults over 50 are at particular risk for sciatica because the structures that support your spine naturally age. Discs lose water content, vertebrae develop bone spurs, and the spinal canal may narrow. Any of these changes can irritate the sciatic nerve.
The most common causes:
- Herniated (slipped) disc: A spinal disc bulges out of place and presses on nerve roots. This is the single most common cause of sciatica.
- Lumbar spinal stenosis: The spinal canal in your lower back narrows, squeezing the nerves inside. This is very common in over-50s and is often linked to arthritis and bone spurs.
- Degenerative disc disease: Over time, the discs that cushion your vertebrae break down, losing height and flexibility. This can allow vertebrae to shift and irritate nearby nerves.
- Spondylolisthesis: One vertebra slips forward over another, pinching nerve roots.
Other causes and risk factors:
- Pregnancy (due to pressure on the sciatic nerve and posture changes)
- Spinal tumours or infections (rare)
- Prolonged sitting or sedentary lifestyle
- Heavy lifting or repetitive bending, especially in physically demanding jobs
- Poor posture
- Muscle tightness in the gluteal region
- Trauma or injury to the spine
Age is the strongest risk factor. As you move through your 50s, 60s, and beyond, your discs naturally deteriorate. This is not a sign that something is wrong with you-it’s normal ageing of the spine. However, it does increase your chance of developing sciatica.
How Sciatica Is Diagnosed: What Your GP Will Do
Diagnosis begins with your GP. Be prepared to describe your pain in detail: where it hurts, when it started, what makes it better or worse, and whether you’ve had any injury or trauma.
Your GP will then:
- Examine your back, hips, and legs
- Test your strength, flexibility, sensation, and reflexes
- Check for signs of nerve compression (such as weakness or loss of feeling)
- Ask about your work, hobbies, and posture habits
Most cases of sciatica are diagnosed based on symptoms and physical examination alone. However, your GP may order imaging to confirm the underlying cause:
- X-rays: Show bone structure and alignment; useful for detecting bone spurs or spondylolisthesis.
- MRI scan: Provides detailed images of soft tissues (discs, nerves, ligaments). This is the best test for identifying a herniated disc or spinal stenosis.
- CT scan: An alternative if MRI is not suitable (e.g., if you have a pacemaker).
- Nerve conduction studies: Rarely needed, but used if your GP suspects other nerve problems.
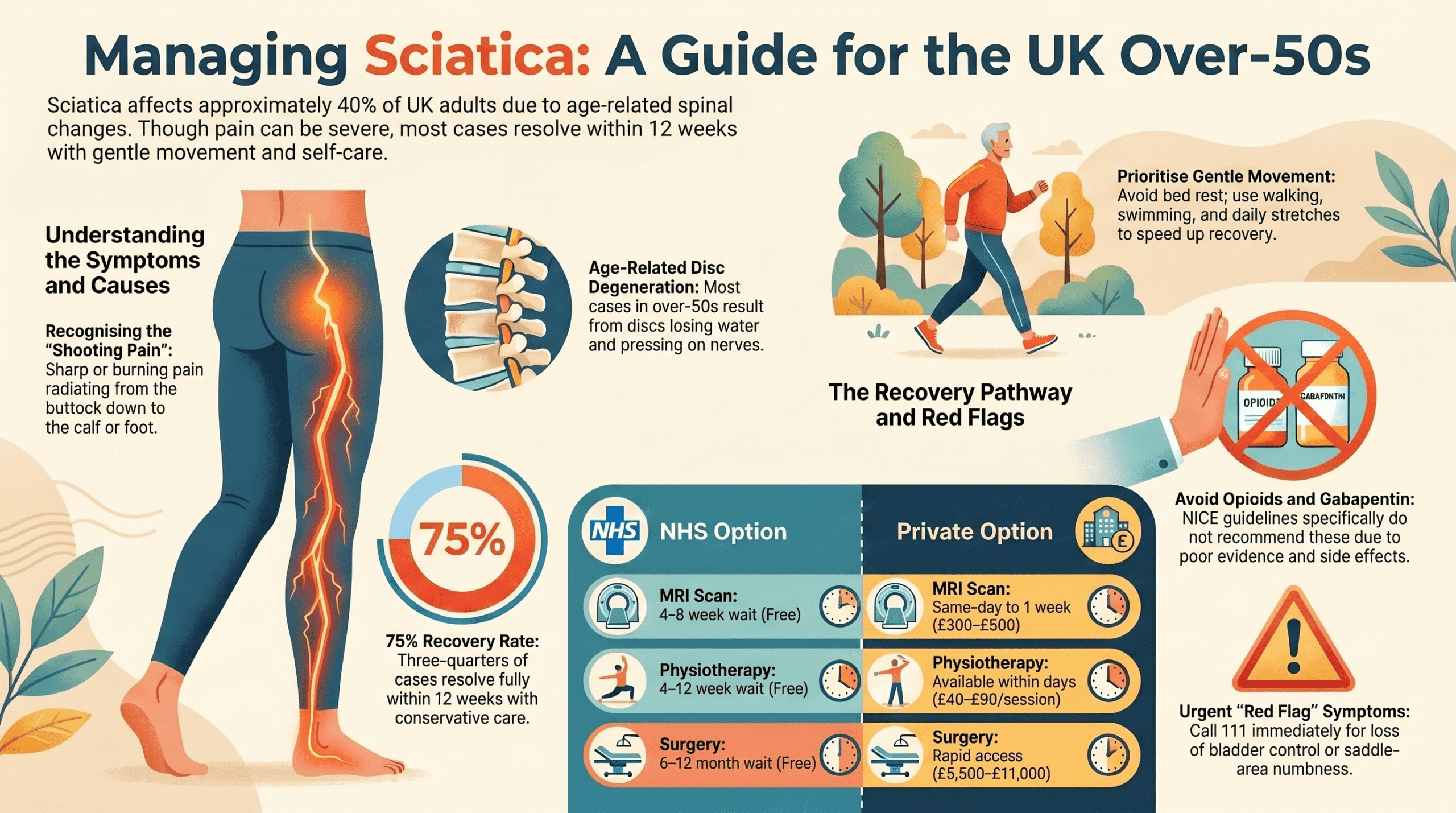
NHS waiting times for MRI scans vary by region but typically range from 4-8 weeks. Private MRI scans can be done within a few days and cost £300-£600 .
When to See Your GP Urgently
In most cases, sciatica is not an emergency. However, seek urgent GP advice (same day) or call 111 if you experience:
- Sudden loss of bladder or bowel control
- Numbness or pins and needles in the genital area or around the anus
- Severe pain combined with high fever (suggests infection)
- Sciatica after a serious fall or injury
- Progressive weakness in your legs
These symptoms may indicate cauda equina syndrome, a rare but serious condition where multiple nerve roots are severely compressed. Early surgery can prevent permanent damage, so don’t delay.
NHS vs Private Sciatica Treatment: Costs and Waiting Times
Your treatment pathway-and the speed of it-depends on whether you choose NHS care or go private. Both routes are valid. Here’s how they compare:
| Treatment | NHS Wait Time | NHS Cost | Private Cost | Private Wait Time |
|---|---|---|---|---|
| GP Consultation | 1-2 weeks | Free | £40-£150 | Same day – 2 days |
| Physiotherapy (6 sessions) | 6-12 weeks wait; 6 sessions free | Free | £240-£480 (£40-£80 per session) | 1-2 weeks |
| Epidural Steroid Injection | 8-16 weeks; often 1 injection | Free | £300-£600 per injection | 1-4 weeks |
| MRI Scan | 4-8 weeks (regional variation) | Free | £300-£600 | 1-4 days |
| Spinal Surgery (discectomy/decompression) | 3-6 months on waiting list | Free | £8,000-£15,000 | 2-6 weeks |
Key takeaway from the table: If you’re in pain and can afford private care, the speed advantage is real. You can see a private physio within days rather than waiting 8-12 weeks on the NHS. However, most people recover with physio alone, so rushing to private surgery is rarely necessary.
The NHS always starts conservatively: first GP assessment, then physio, then injections if physio hasn’t worked, and surgery only as a last resort. Private providers may move faster through these stages, but they’re not necessarily more effective.
Sciatica Treatment Options: Step by Step
Step 1: Initial Pain Management and Anti-Inflammatory Treatment
Your first line of treatment focuses on reducing inflammation and pain while you await physio or further investigation.
- Over-the-counter NSAIDs: Ibuprofen (e.g. Nurofen) or naproxen (e.g. Naproxen) reduce inflammation and pain. Typical dose is 400-600 mg of ibuprofen, three times daily with food. These work best in the first 1-2 weeks of acute pain.
- Prescription NSAIDs: If over-the-counter doses aren’t enough, your GP can prescribe stronger NSAIDs such as indomethacin or meloxicam.
- Oral steroids: A short course of oral corticosteroids (e.g. prednisolone) may be prescribed for severe inflammation, though this is less common than NSAIDs.
- Hot or cold compression: Apply a heating pad for 15-20 minutes to soothe muscle tightness, or an ice pack for 10-15 minutes to reduce acute inflammation. Alternate based on what feels better for you.
Always take NSAIDs with food to protect your stomach, and discuss them with your GP if you have a history of gastric ulcers or take blood thinners.
Step 2: Physiotherapy and Exercise
Physiotherapy is the cornerstone of sciatica recovery. A physiotherapist will assess your posture, movement patterns, and muscle strength, then guide you through targeted exercises to relieve nerve compression and prevent future flare-ups.
NHS referrals typically come from your GP. You may wait 6-12 weeks for an appointment, and the NHS usually funds 6 sessions. Private physios can be seen within 1-2 weeks and offer more frequent sessions if desired.
Step 3: Epidural Steroid Injections
If physio and NSAIDs haven’t reduced pain within 4-6 weeks, your GP may refer you for an epidural steroid injection. A consultant radiologist or pain specialist guides a needle to the source of nerve inflammation and injects steroid directly around the nerve roots.
The injection provides 4-12 weeks of relief, giving physio time to work. Most people need only one injection; some may have two or three spaced weeks apart.
NHS route: Referral from GP to pain clinic or radiology. Wait 8-16 weeks. Cost-free.
Private route: Book directly with a private pain clinic or sports medicine doctor. Cost £300-£600 per injection , available within 1-4 weeks.
Step 4: Surgery (Discectomy or Decompression)
Surgery is reserved for cases where conservative treatment has failed and pain remains severe after 6-12 weeks. The goal is to remove the disc material or bone spurs that are compressing the nerve.
Microdiscectomy: Minimally invasive removal of a herniated disc. Recovery takes 4-6 weeks.
Laminectomy (decompression): Removal of part of the vertebral bone to widen the spinal canal, often used for spinal stenosis. Recovery takes 6-12 weeks.
NHS route: Referral from GP to spinal surgeon. Wait 3-6 months. Surgery is free, but you’ll need to wait for a bed.
Private route: Book directly with a private spinal surgeon. Cost £8,000-£15,000 , surgery within 2-6 weeks.
Most people recover without surgery. Only 5-10% of sciatica cases require an operation. Surgery is most effective when there is clear structural compression (e.g. a large herniated disc) and significant, unrelenting pain.
Self-Help Sciatica Exercises and Pain Relief
Physiotherapists recommend gentle, progressive exercises to strengthen your back and stretch tight muscles. If you are managing pain that goes beyond a typical sciatica episode, our guide on chronic pain and exercise covers gentle activity strategies for over-50s. The key is gradual progression-never force an exercise if it causes sharp pain. Mild discomfort during stretching is normal; sharp, radiating pain means you’ve gone too far.
Perform these exercises 5-6 days per week, holding each stretch for 30 seconds. If any exercise makes your sciatica worse, stop and consult your physio.
Standing Hamstring Stretch
This stretch targets the back of your thigh and calf, relieving tension that can irritate the sciatic nerve.
- Stand facing a step, low stool, or sturdy chair.
- Place your right foot on the elevated surface, keeping your leg straight.
- Flex your toes upward.
- Hinge forward at your hips, bending slightly until you feel a gentle stretch down the back of your leg.
- Hold for 30 seconds.
- Repeat 3 times on each leg.
Sitting Spinal Twist Stretch
This stretch mobilises your spine and relieves pressure on the sciatic nerve roots.
- Sit on the ground with your legs stretched out straight in front of you, toes flexed upward.
- Bend your right knee and place your right foot flat on the floor outside your left knee.
- Place your left elbow on the outside of your right knee.
- Gently turn your upper body to the right, using your elbow against your knee for leverage.
- Hold for 30 seconds.
- Repeat 3 times, then perform the same stretch on the opposite side.
Reclining Pigeon Pose
This deep hip stretch targets the piriformis muscle, which can compress the sciatic nerve when tight.
- Lie on your back with both knees bent and feet flat on the floor.
- Lift your right leg and place your right ankle on top of your left knee, creating a figure-four shape.
- Clasp both hands behind your left thigh and gently pull your left leg toward your chest.
- Feel the stretch in your right buttock and hip.
- Hold for 30-45 seconds.
- Release and repeat 3 times on each side.
Seated Pigeon Pose
A gentler alternative to the reclining version if you have difficulty lying down.
- Sit on the floor with both legs stretched in front of you.
- Bend your right knee and place your right ankle on top of your left knee.
- Lean your upper body forward toward your thighs, keeping your spine long.
- Feel the stretch in your right hip and buttock.
- Hold for 15-30 seconds.
- Repeat 3 times on each side.
Pelvic Tilts (Strengthening)
Strong core and lower back muscles support your spine and prevent future sciatica flare-ups.
- Lie on your back with knees bent and feet flat, hip-width apart.
- Tighten your abdominal muscles and press the small of your back into the floor.
- Hold for 5 seconds, then relax.
- Repeat 10-15 times, rest, and do another set.
Walking
Regular walking is one of the safest and most effective exercises for sciatica. Aim for 20-30 minutes daily on flat ground. Walking improves circulation, strengthens your back, and rarely aggravates sciatica-unlike sitting or bending forward.
Important: If any exercise sharply increases your pain or radiates further down your leg, stop immediately and consult your physiotherapist or GP.
Prevention: Avoiding Future Sciatica
Once you’ve recovered from sciatica, preventing a recurrence is crucial. Sciatica prevention sits within broader healthy ageing – see our guide on healthy living for longer lives. Most people who don’t address underlying weakness or posture issues will experience another flare-up within 1-2 years.
Posture at work: If you have a desk job, invest in an ergonomic chair with lumbar support. Keep your feet flat on the floor and monitor at eye level. Stand and walk every 30-60 minutes.
Lifting technique: Always bend at your knees and hips, not your waist. Keep heavy objects close to your body. Never twist your spine while holding weight.
Regular exercise: Aim for 150 minutes of moderate activity weekly (walking, swimming, cycling). Include core-strengthening exercises 3 times per week.
Stretching: Spend 10 minutes daily stretching your hamstrings, hip flexors, and piriformis muscle. This prevents muscle tightness that can lead to sciatica.
Weight management: Extra weight increases pressure on your lower back and discs. Maintaining a healthy weight reduces your sciatica risk.
Avoid prolonged sitting: If your job requires long hours at a desk, use a stand-up desk part of the day, take walking breaks, and adjust your seat regularly.
Sleep posture: Sleep on your side with a pillow between your knees, or on your back with a pillow under your knees. Avoid sleeping on your stomach.
Questions to Ask Your GP About Sciatica Treatment
When you see your GP, take notes and ask these questions to make informed decisions about your care:
- What do you think is causing my sciatica? Do you need imaging to confirm?
- Can I start physiotherapy now, or do I need to wait for imaging results?
- How long should I expect to feel better? What’s the typical timeline?
- Are there any NSAIDs you would recommend, and for how long should I take them?
- If physio doesn’t help within 4-6 weeks, what’s the next step?
- Am I a candidate for an epidural steroid injection? What are the risks?
- When would surgery be considered, and what would it involve?
- Are there any red flags I should watch for that would need urgent attention?
- Can you refer me to an NHS physio, or should I consider private treatment to get started faster?
- Are there any activities I should avoid while recovering?
Write these down and bring them to your appointment. A good GP will take time to explain your options and involve you in shared decision-making.
The Outlook: Recovery and Long-Term Management
The prognosis for sciatica is good. For another lifestyle change that pays dividends after 50, see our guide on how to lower your blood pressure naturally. Most people recover within 4-12 weeks with conservative treatment (physio, NSAIDs, time). Permanent nerve damage is rare.
However, sciatica tends to recur if you don’t address the underlying cause and maintain good posture and core strength. After recovery, ongoing stretching and exercise are essential to prevent another flare-up.
If you’re in significant pain, don’t assume you must endure months of suffering waiting for NHS physio. Private physiotherapy is affordable (£40-£80 per session) and can get you started within days. Many people find that a few weeks of intensive private physio significantly accelerates their recovery, allowing them to return to normal activities sooner.
Frequently Asked Questions
What is sciatica and what does it feel like?
Sciatica is pain caused by irritation or compression of the sciatic nerve, which runs from the lower back down each leg. It usually feels like a sharp, burning, or shooting pain that radiates from the buttock down the back of the thigh and sometimes into the calf or foot. The NHS estimates around 40 per cent of UK adults experience it at some point in their life.
How long does sciatica typically last?
Most cases of sciatica improve within 4 to 6 weeks with self-care, gentle movement, and over-the-counter pain relief. Around 75 per cent of cases resolve fully within 12 weeks. If pain persists beyond 6 weeks or worsens, your GP may refer you to physiotherapy or for imaging.
Should I rest or keep moving with sciatica?
NHS guidance is clear: gentle, regular movement helps recovery. Long-term bed rest actually slows healing and can worsen stiffness. Walk short distances, do light stretching, and avoid sitting for more than 30 minutes at a time. Your physiotherapist can give you specific exercises to do daily.
When should I see a GP urgently for sciatica?
Call 111 or your GP urgently if you develop loss of bladder or bowel control, numbness around the genitals or inner thighs (saddle anaesthesia), severe weakness in both legs, or sciatic pain following a fall or trauma. These are red-flag symptoms of cauda equina syndrome – a rare but serious condition needing emergency assessment.
Will sciatica need surgery?
Surgery is uncommon – around 5 per cent of UK sciatica patients eventually need it. NHS surgery (microdiscectomy or laminectomy) is reserved for cases where conservative treatment has failed for more than 6 to 12 weeks, or where there are red-flag neurological symptoms. Most over-50s recover fully without surgery.
Can private treatment speed up sciatica recovery?
Private MRI scans (around £300 to £800) can confirm a diagnosis within a week rather than NHS waits of 4 to 8 weeks. Private physiotherapy (typically £40 to £90 per session) is available within days. For most over-50s, the bottleneck is imaging and physio access – both can be accelerated privately if NHS waits are too long.
Useful Resources and Sources
For more detailed, evidence-based information on sciatica, consult these trusted UK and international organisations:
- NHS.uk – Sciatica: https://www.nhs.uk/conditions/sciatica/ – Comprehensive information on diagnosis, treatment, and when to seek help.
- NICE Guidelines – Low Back Pain and Sciatica: https://www.nice.org.uk/guidance/ng59 – Evidence-based clinical guidelines for treatment pathways.
- Chartered Society of Physiotherapy (CSP): https://www.csp.org.uk/ – Find accredited physiotherapists and evidence on physio for back pain.
- Versus Arthritis – Sciatica and Lower Back Pain: https://www.versusarthritis.org/ – Information on back pain, self-management, and lifestyle changes.
- BackCare – The Charity for Healthier Backs: https://www.backcare.org.uk/ – Resources on posture, exercise, and back pain prevention.
- Spine-health.com – Sciatica Treatment: https://www.spine-health.com/ – Detailed, physician-reviewed information on causes and treatment options.
Summary: Sciatica Causes and Treatment at a Glance
Sciatica is a symptom of nerve compression, most often caused by a herniated disc, spinal stenosis, or degenerative disc disease. It is more common in over-50s due to natural spine ageing.
Most people recover within 4-12 weeks using conservative treatment: physiotherapy, NSAIDs, and gradual return to activity. Surgery is rarely needed-reserved for persistent, severe cases.
You have a choice: start with the free NHS pathway (waiting 6-12 weeks for physio), or invest in private physiotherapy (£40-£80 per session, available immediately). Many people benefit from a combination: private physio to get fast relief, then ongoing NHS follow-up.
The key to recovery and prevention is consistent exercise, good posture, and patience. Your sciatic nerve will likely feel better-often without any intervention beyond rest and gradual movement.
If you experience warning signs (sudden bladder/bowel loss, progressive leg weakness, severe unrelenting pain), seek urgent GP or emergency care immediately.
Next Steps: Take Action on Your Sciatica Recovery
Don’t wait in pain. If you’re experiencing sciatica symptoms:
- Book a GP appointment this week. Describe your pain and ask for an NHS physio referral or a private physio recommendation.
- Start the stretches above today. Gentle movement often brings immediate relief. Avoid sitting for long periods.
- Consider your pathway. If NHS waiting times are long in your area, private physio is affordable and effective. A few sessions may speed your recovery significantly.
- Join our community. Follow The Best of Health on Facebook for tips on back health, exercises, and updates on NHS vs private healthcare costs and waiting times for over-50s in the UK.
Sciatica is painful, but it is treatable. With the right support and consistent effort, you will recover.
Disclaimer
This article is for information only. It is not a substitute for professional medical advice. Always consult your GP or a qualified healthcare professional before making health decisions, starting new exercises, or changing your treatment plan. If you experience warning signs such as loss of bladder or bowel control, progressive weakness, or severe unrelenting pain, seek urgent medical attention.









