 Diverticulitis is one of the most common health problems of this century in the Western world and one which is increasingly common in the over 50s. It causes severe abdominal pain, nausea and bloating but you might be able to avoid it.
Diverticulitis is one of the most common health problems of this century in the Western world and one which is increasingly common in the over 50s. It causes severe abdominal pain, nausea and bloating but you might be able to avoid it.
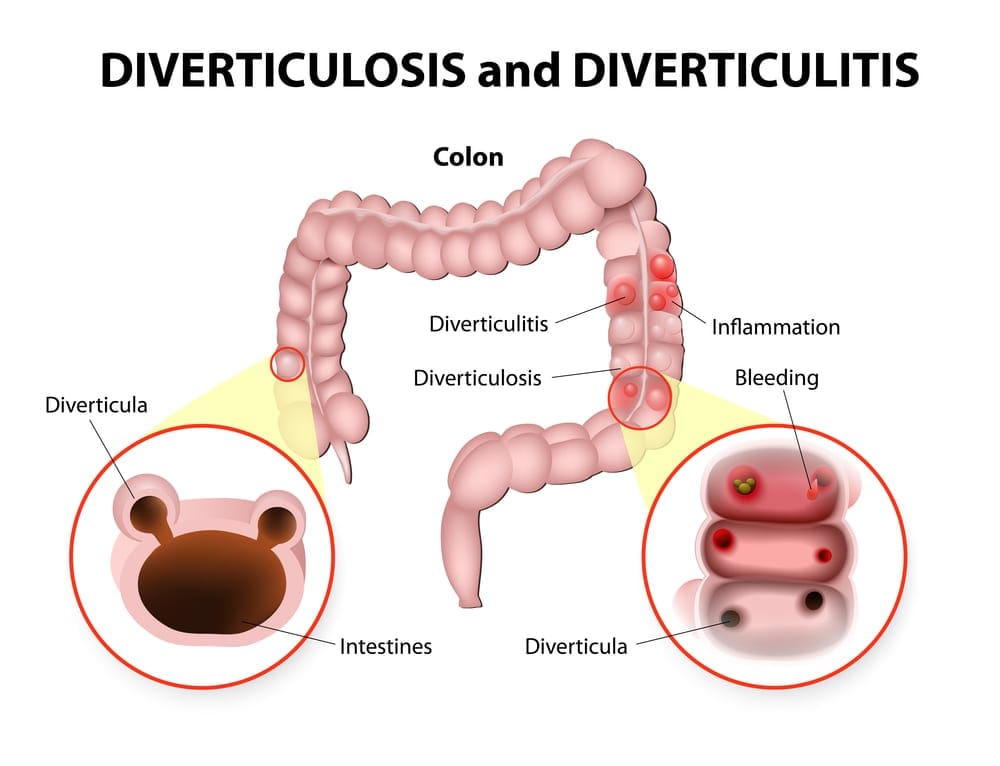
Diverticulitis – sometimes referred to as diverticular disease, is a medical condition that affects the colon (large intestine). When you suffer from it, small bulges that form within the lining of the intestine have become infected or inflamed.
When this happens you can feel unduly bloated or even suffer pain in the lower abdomen. Often, if you have these bulges in the colon but you are not suffering due to infection, you may feel nothing. However, if your temperature rises and you feel pain and notice that you are having more frequent trips to the toilet or even have diarrhoea, then diverticulitis may be the problem.
How do we get diverticulitis?
Many of us can suffer from diverticula i.e. the bulges in the colon, as we get older. The large intestine gradually weakens and large stools being forced through with difficulty can create these bulges. If these bulges form but don’t become inflamed and cause any problems, then the condition is called diverticulosis. Statistics show that by the time we hit 40, 5% of us have these diverticula and by the age of 80, 50% of people may have them.
But this does not mean that you will suffer from diverticulitis i.e. disease of the diverticula. This occurs when bacteria from trapped stools get inside the bulges in the colon, triggering complications. Left untreated, this can even result in the forming of abscesses.
What can we do to help?
Whilst we may not be able to prevent diverticula forming as we get older, we can do a lot to help by eating a high fibre diet. If you have mild pain, standard pain killers such as paracetamol can help; don’t use aspirin or ibuprofen as these may irritate the stomach even more. If you do end up with mild diverticulitis then your doctor will normally prescribe antibiotics.
Hospital treatment will only be required if complications develop and at this point, surgery to remove the infected section of the intestine may be considered.
You may hear diverticulitis referred to as a very ‘Western disease’ as our rates are much higher than in Africa or Asia. This is due to genetics and the fact that we tend to eat less fibre. If you are over 50 and eat at least 25g of fibre each day, you can reduce your risk of diverticulitis by 40%.

Why fibre?
Eating plenty of fibre helps the body’s digestive process and keeps stools soft and well formed, avoiding things such as constipation. When you digest soluble fibre, it makes sure that more water is retained when the body forms stools. They will pass through the intestines a lot more easily and prevent you feeling bloated, sluggish and uncomfortable.
Low fibre diets are not recommended because they can cause constipation. When this occurs, your body has to apply more pressure to try and evacuate the stool and this may further add to creation of the diverticula.
Infections occur when portions of stool get trapped in these ‘pockets’ or bulges; severe cases are referred to as non-inflammatory stricture and may require surgery to remove the diverticula that is causing the problem. If this happens often and scarring forms in the bowels, blockages and obstructions in the colon may occur; this is a serious and life-threatening event as the intestine may rupture, ending with peritonitis.
Change your diet

If you are not sure where to get your fibre from, try adding to your diet plenty of fresh and dried fruit, vegetables, nuts, cereals and brown bread, rice or pasta. Don’t go mad but increase your fibre intake gradually so that bloating and wind do not result. Also drink plenty of fluids. If for some reason you cannot do this, you can add fibre supplements in the form of powders mixed with water, available from chemists.
Once you have improved your diet, stick with it, particularly as you age. Low-fibre foods may not make your diverticulitis any worse, but try not to consume too many. Here are a few examples of foods to try and avoid:
- canned fruit or vegetables
- eggs
- fish
- poultry
- refined white flour and bread
- fruit juice without pulp
- cereals low in fibre
- dairy products
It used to be the case that when people found they had diverticula in the lining of their colon, they would be told not to eat things like popcorn, seeds and nuts as they may lodge in the pouches or bulges. However, there is no real evidence to support this so unless you find that these foods trigger pain, they should be fine to eat.
Other diverticulitis triggers
Other factors, as well as a low fibre diet, can cause diverticulitis or diverticular disease. These include consuming excessive alcohol, being overweight and smoking. Things such as fizzy drinks, too much tea and coffee, chocolate and caffeinated drinks, can all irritate the intestine.
Caffeine in particular can make your colon contract, making the muscles eliminate water from the body. This causes us to dehydrate and is not good. This water is needed to form soft stools and thus avoid constipation. For this very reason, drinking plenty of water is essential at all times.
So as you can see, whilst we may not be able to avoid diverticula occurring in the colon, we can do a lot to prevent them worsening or getting infected. Lots of fibre in the diet is required to keep the bowels working easily and reducing the stress on the intestines. This way, even if we acquire a few bulges and pockets in the colon as we age, they should not cause great problems.
It is only when we fail to take care of our diet and irritate the bowel by consuming large amounts of caffeine, alcohol or smoking that diverticulitis can become a real problem.
If you feel that your abdomen is tender and you feel sick, bloated and are passing stools or urine frequently, then you need to visit your doctor or medical centre to see if diverticulitis may be at the root of the problem.
The UK Charity GutsUK may be able to offer further help and advice if you suffer from diverticulitis or other digestive disorders such as crohn’s disease, coeliac disease or irritable bowel syndrome (IBS).
If you think this information may benefit a friend or relative, don’t hesitate to Share it via the links below.
Finally, if you suffer from diverticulitis and would like regular updates on this and other over 50s health conditions, please follow us on Facebook or sign up to our free newsletter.









