
Ulcerative colitis is a chronic condition that causes inflammation and ulceration of the inner lining of the large intestine. The large intestine or colon removes nutrients from food and gets rid of waste products through the rectum and anus when we pass stools. In ulcerative colitis, tiny ulcers develop on the lining of the colon. These are painful, may bleed and produce pus and mucus. It is a fairly common condition thought to affect 100,000 people in the UK and between 250,000 and 500,000 people in the USA.
It is one of the two main forms of Inflammatory Bowel Disease or IBD. The other is Crohn’s disease.
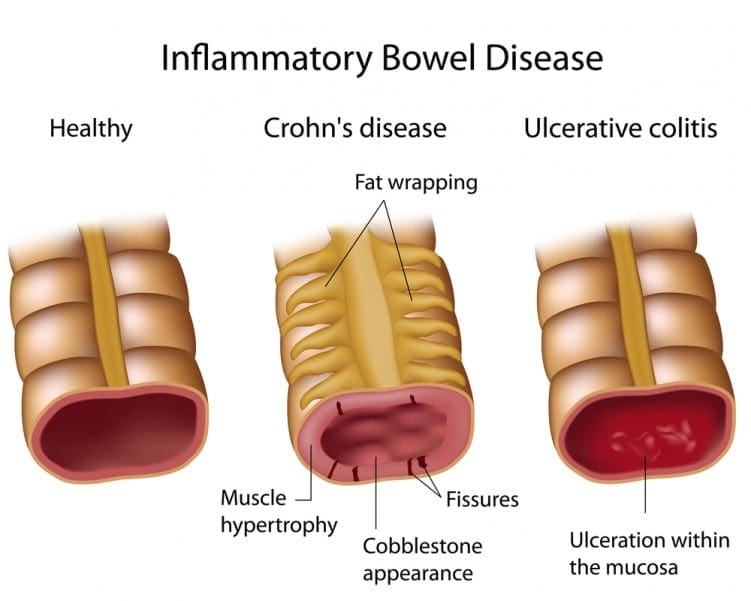
What are the symptoms of ulcerative colitis?
Symptoms may vary from person to person but the most common are:
- Abdominal pain
- Diarrhoea
- Cramping pain in the abdomen
- Loss of appetite
- Weight loss
- Fatigue or tiredness
- A high temperature and fever
- Anaemia
- Dehydration
- Rectal bleeding
As with other chronic conditions, ulcerative colitis is on-going and life-long. You may have periods of remission or good health followed by relapses or flare-ups of your symptoms.
What are the causes of ulcerative colitis?
Although the causes of ulcerative colitis are not well understood, research suggests that gut bacteria may play an important role. Genetics, the environment and the body’s own immune system are also thought to be involved:
- About one in five patients have a close relative with the disease. New research has identified a faulty gene which appears to be linked to ulcerative colitis.
- Contributory factors in the environment are thought to include diet, cigarette smoke, air pollution, viruses and hygiene.
- The inflammation may be caused by the body’s response to a viral or bacterial infection in the intestine.
- A high intake of linoleic acid is also thought to be linked to the condition. This is a common dietary fatty acid and can be found in red meat, some cooking oils and margarines.
What treatments are there for ulcerative colitis?
Treatment depends on the severity of your symptoms and aims to induce and maintain remission.
Many of the drugs used are anti-inflammatory drugs such as aminosalicylates (5ASAs). These can be used in the short term for flare-ups or can also be taken for the rest of your life to maintain remission.
Corticosteroids are a more powerful form of medication and can be used if 5ASAs aren’t effective. However, the possible side effects prevent them from being used in the long term. These side effects include osteoporosis (weakening of the bones) and cataracts. Short term side effects include acne, weight gain, insomnia and mood changes.
Immunosuppressants, which reduce the activity of the immune system, can be very effective in treating ulcerative colitis but often take two to three months to start working.
Biological drugs such as infliximab or adalimumab may be used to treat more severe symptoms. They target and block proteins which the immune system uses to stimulate inflammation.
Surgery may be an option if your flare-ups have a significant effect on your quality of life. This involves permanently removing the colon. Your small intestine will then take over the role of passing waste products out of your body. The most common surgery involves an internal pouch, known as a J-pouch or ileo-anal pouch, being created. Part of the small intestine is connected to the anus allowing you to pass stools normally. However, you must consider the risks of surgery before opting for this form of treatment.
Your GP and specialist team will advise you as to the most effective treatment plan for your particular symptoms.
Living with ulcerative colitis
Living with any chronic condition can be a challenge. When you are well, you may live life to the full. But during flare-ups you may have to make adjustments and take things easy. The following strategies may help you maintain your overall health and wellbeing:
- Build up a good relationship with your GP and medical team to get the best out of your care.
- Open up about your condition to work colleagues, family and friends so they understand when you are feeling unwell and are more able to give you the support you need.
- Eat a nutritious and balanced diet. During flare-ups it may be advisable to eat bland, soft foods and keep off raw vegetables, spicy foods and foods which are high in fibre.
- Drink sufficient liquid to stop you getting dehydrated.
- Try to come to terms with your condition and accept that, at times, you may need to make adjustments in your life.
- Find out as much as you can about your condition and think about joining a forum such as Health Unlocked.
- Take your prescribed medication on a regular basis to reduce the chance of a flare-up and the need for stronger drugs such as steroids.
- Be careful with hygiene when preparing food and take extra care when travelling abroad.
- Try to lower your stress levels and make time for relaxation each day.
- Take regular exercise to improve your overall health and reduce the risk of muscle weakness and stiff joints.
A new study into the use of vinegar in the treatment of ulcerative colitis
Researchers led by Jilin University in Changchun, China have found that vinegar appears to suppress inflammatory proteins and also increase beneficial bacteria in the guts of mice. The study was published in the Journal of Agricultural and Food Chemistry.
The vinegar and it’s main ingredient acetic acid, was added to the drinking water of mice which had been bred to develop symptoms of ulcerative colitis. After a month the researchers found that the mice had higher levels of friendly bacteria in their gut such as Lactobacillus and Bifidobacteria. Other studies have shown that these bacteria are beneficial for colitis. Inflammation in the colon was also reduced as the vinegar suppressed proteins and molecular processes that trigger inflammation.
The researchers also found that vinegar appears to reduce a type of cell death that is triggered by stressful conditions.
Further studies will be needed to establish if the results of their findings are true of humans.
If you would like more advice and help on Crohn’s or ulcerative colitis please click on the link to the UK society for the conditions https://www.crohnsandcolitis.org.uk/
Finally, if you have found this article helpful and you know someone else who may benefit from it, please share it with them.









